It should be considered a clue to the presence of one or several underlying disorders, including prothrombotic disorders, whether or not a local. John tan, 20 years in vein care

Treatment of portal vein thrombosis.
Portal vein thrombosis treatment. Portal vein thrombosis (pvt) is increasingly frequently being diagnosed, but systematic descriptions of the natural history and clinical handling of the condition are sparse. If a blood clot suddenly blocks the vein, a drug that dissolves clots (such as tissue plasminogen activator) is sometimes used. John tan, 20 years in vein care
Compelling evidence from one prospective trial treating patients without pvt with prophylactic lmwh showed that prevention of pvt is associated with decreased hepatic decompensation and improved survival. Ad one stop center for thrombosis dr. Outline the scenarios of portal vein thrombosis.
Enoxaparin prevents portal vein thrombosis and liver decompensation in patients with advanced cirrhosis. Portal vein thrombosis (pvt) is being increasingly diagnosed in patients both with and without cirrhosis, as contrast enhanced imaging has continued to evolve and improve. Patients with nonbleeding varices and pvt should be anticoagulated in the hope of recanalization of the portal vein.
Venous thrombosis are more common than arterial ones [1,2]. To assist health care professionals in the management of portal vein thrombosis (pvt). Treatment of portal vein thrombosis.
Mechanisms leading to thrombosis are still unclear [1]. However, there are data to support treatment of specific patients with anticoagulation agents. We review the common and distinct features of portal vein thromboses in patients without liver tumors, with and without cirrhosis.
Newer oral anticoagulants are safe and efficacious alternatives to traditional anticoagulation with low molecular weight heparin and vitamin k antagonists in the treatment of acute portal vein thrombosis with or without cirrhosis. If the patient is imaged and a partial thrombosis of the portal vein is found, i would anticoagulate to avoid completion of the process and the onset of symptoms. The portal vein is formed by the confluence of the splenic and superior mesenteric veins, which drain the spleen and small intestine, respectively ().occlusion of the portal vein by thrombus (portal vein thrombosis [pvt]) typically occurs in patients with cirrhosis and/or prothrombotic disorders ().chronic pvt develops in patients with acute pvt.
Lmwh, vka antibiotics (if evidence of phlebitis) interventional therapies tips tips transjugular/transhepatic thrombolysis surgical thrombectomy Treatment of portal vein thrombosis is done by treating the underlying cause. Warfarin, lmwh, or doacs are agents of choice for anticoagulation.
Portal vein thrombosis (pvt) can be a difficult clinical problem to assess and manage. Medication for acute pvt, doctors commonly recommend. In one study in which 84 of 136 nonmalignant, noncirrhotic patients with portal vein thrombosis were anticoagulated with similar bleeding risks but less risk for thrombotic propagation.
Treatment of portal vein thrombosis. Portal vein thrombosis is an unusual thrombotic condition not frequently seen in the general population; Portal venography usually is unnecessary unless a surgical portosystemic shunt is being considered.
For portal vein thrombosis, treatment recommendations will focus on dissolving the blood clot or preventing growth over a long period of time. When the diagnosis of portal vein thrombosis is still uncertain, magnetic resonance angiography is better than ct in demonstrating the typical changes of portal vein thrombosis (portal cavernoma) ( fig. John tan, 20 years in vein care
Anticoagulation therapy has also been recommended after shunt surgery to prevent rethrombosis. Medications may be given to dissolve the clot and restore normal blood flow. It should be considered a clue to the presence of one or several underlying disorders, including prothrombotic disorders, whether or not a local.
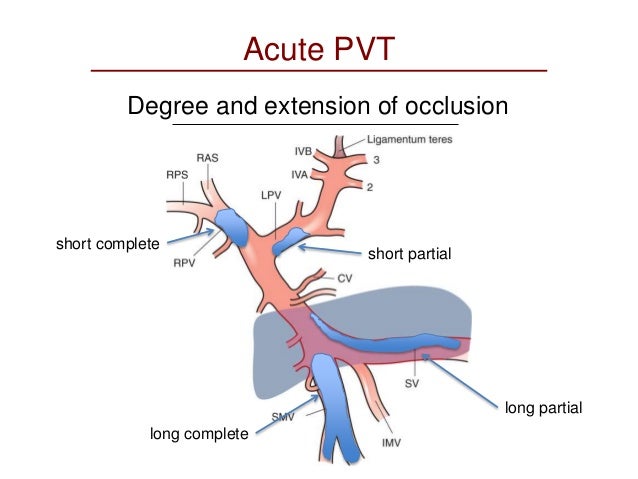
Management of portal vein thrombosis in patients with cirrhosis is more controversial. Scenarios and principles of treatment andrea de gottardi, hepatology, inselspital, university of berne. Pvt can occur in the main portal vein, in the left or right portal branches and/or in the smaller,.
Anticoagulation therapy duration should be tailored to the identified predisposing factors. Drugs (to dissolve or prevent blood clots) treatment of cause of blockage and complications. Medical and interventional therapies for acute and chronic portal vein thrombosis pvt acute chronic medical therapies anticoagulation:
1 thrombosis of the portal vein is an uncommon disorder comprising of thrombosis of the extrahepatic portion of the portal vein and/or its branches. The portal vein is one of the splanchnic veins, formed at the confluence of the superior mesenteric and splenic veins and carries blood from the gastrointestinal tract to the liver. However, it has a higher prevalence in special circumstances such as in liver cirrhosis and hepatic or pancreatic malignancy.
However, chronic pvt should be treated conservatively with measures to control major consequences related to portal hypertension. The portal vein represents the confluence of the splenic (drains the spleen) and superior mesenteric veins (drains the small bowel). The effectiveness of this treatment (called thrombolysis) is unclear.
In some cases angiography may be done so that blood can go to the liver through an alternate route. It can occur concomitantly with. It originates posterior to the pancreas by the confluence of superior mesenteric and splenic veins, and, prior to entering into the liver, it divides into the left and right portal vein.
The most frequent localization is hepatic veins (40%) (2) leading to budd chiari syndrome but other abdominal sites like portal, mesenteric and splenic thrombosis are less frequently affected in addition to cerebral thrombosis [1]. Ad one stop center for thrombosis dr.